|
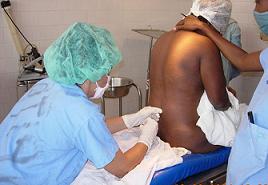
Spinal AnesthesiaSpinal anesthesia is performed by the injection of a local anesthetic solution into the spinal sac, typically below the level of the spine where the spinal cord ends and becomes a large group of nerves encased in this sac.
This type of anesthesia is very beneficial, and frequently used for surgical procedures below the umbilicus (belly button) including the lower abdomen and extremities. Spinal anesthetics are typically not used for procedures of the upper abdomen or higher, because anesthetics of this nature will paralyze the diaphragm and disrupt breathing.
Examples of agents used include Marcaine, Tetracaine, Xylocaine and Sensorcaine. Each agent has a different effect upon the spinal nerves it comes in contact with; creating "blocks" of varying lengths of duration. These effects can range from a very short acting block (approximately 30 minutes), to one that can last several hours. Unlike epidural anesthetics, spinal anesthetics are a "one-shot" anesthetic and will eventually wear off. Therefore, these blocks are typically used in procedures with very definite time frames.
The anesthetic agent wears off slowly, so post operative pain returns slowly, thus allowing for better pain management and erarlier institutiom of oral analgesics (pain medications). The patient does not have to be rendered unconscious and be intubated (endotracheal tube). The ability to add narcotic pain medication to the anesthetic injection for extended pain relief.
Risk of “post-puncture” headaches (much less likely than in years past) Paralysis of the diaphragm if spinal too “high” Potential for hypotension (low blood pressure) with “high” spinals
Leave Spinal Anesthesia; return to Home Page
|

"We hope you enjoy your journey through Bone and Joint Pain.com"